Breakthrough brain implant successfully treats seizures and OCD
A patient has become the first person ever to receive a single brain implant, designed to manage both epilepsy-induced seizures and OCD.
[Oct. 29, 2023: Staff Writer, The Brighter Side of News]
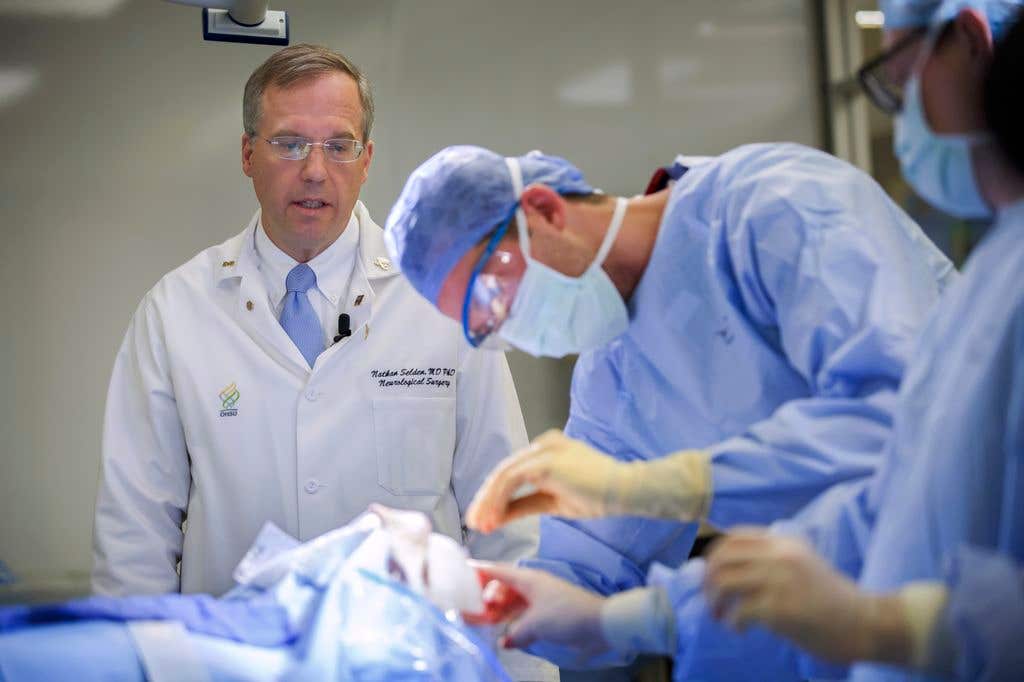
A patient has become the first person ever to receive a single brain implant, designed to manage both epilepsy-induced seizures and OCD.(CREDIT: Oregon Health & Science University)
In a monumental breakthrough at Oregon Health & Science University (OHSU), a patient has become the first person ever to receive a single brain implant, designed to manage both epilepsy-induced seizures and the compulsive behaviors characteristic of obsessive-compulsive disorder (OCD).
The recipient, 34-year-old Amber Pearson from Albany, Oregon, expressed her profound relief, especially concerning her OCD symptoms. “OCD is worse than having the seizures,” she stated. “Epilepsy brings limitations to my life, but OCD controlled it.”
The pioneering technique and its outcomes have been meticulously detailed in a study appearing in the renowned journal Neuron. This paper brings together expertise from esteemed researchers and medical practitioners from various institutions across the U.S.
Amber's struggles with OCD had led her to habits that significantly disrupted her life. She shared, “Before I started treatment with my RNS, I would wash my hands until they would bleed. My hands would be so dry that bending my fingers would crack the skin of my knuckles.”
Related Stories
Additionally, she spent up to 45 minutes nightly checking windows, closets, and the stove. Her fear of contamination was so profound that she couldn’t sit beside others during meals, not even with family during holidays. Even a task as simple as changing her cat's litter box mandated a shower.
This trajectory changed dramatically after a procedure at OHSU on March 5, 2019.
Leading the procedure was Dr. Ahmed Raslan, professor of neurological surgery at the OHSU School of Medicine. While the implant, known as the responsive neurostimulation system (RNS), was primarily aimed at controlling Amber’s seizures, it was strategically placed to span the nucleus accumbens, a critical brain area linked to motivation, action, and compulsive urges. “I could target both portions of the brain and get a second benefit,” Dr. Raslan said of the innovative approach.
OHSU neurosurgeon Ahmed Raslan, M.D., and patient Amber Pearson. (CREDIT: OHSU/Christine Torres Hicks)
Collaboration was key. Raslan partnered with Dr. Casey Halpern, a neurosurgeon at Penn Medicine, who had a role in the research component of the procedure, handling the OCD aspect through Stanford University.
Amber's journey began much earlier, in 2016, when she met Dr. Marissa Kellogg, an assistant professor of neurology at the OHSU School of Medicine. Despite facing significant health challenges, Amber’s proactive mindset stood out. Recalling their first meeting, Dr. Kellogg said, “The first thing she told me when I met her was, ‘I want brain surgery for my epilepsy.’”
NAc-VeP electrophysiology derived from laboratory-based provocation of obsession. Naturalistic provocation task; bottom row: items in VR provocation task. (CREDIT: Neuron
In 2018, Amber underwent a conventional surgical procedure at OHSU targeting drug-resistant seizures. Although successful in curbing some seizures, the method wasn't wholly effective. This led Amber to opt for the RNS implant, a revolutionary device that not only tracks brain activity but also sends tiny pulses to prevent impending seizures. She had read reports of similar implants easing psychiatric conditions, like OCD, and was eager to explore this avenue.
Dr. Kellogg, whose professional interest lies at the intersection of epilepsy and mental health, emphasized Amber's forward-thinking nature. She noted, “Amber is really a future-thinking patient, and she really drove the boat here.”
Postoperative computed tomography (CT) and preoperative magnetic resonance imaging (MRI) were co-registered to localize the rDBS electrode contacts: one electrode contact was located in the posterior border of the right VeP, and the other electrode contact was in the ventral anterior border of the right NAc. (CREDIT: Neuron)
In the months following the implantation of the RNS, Amber reported a noticeable alleviation of her OCD symptoms. Four years post-procedure, the transformation is undeniable. She happily reported, “Now I rarely worry about what’s going on at my house while I’m away. I’m noticing fewer obsessions and compulsions all the time. I’ve been able to form healthier relationships with the people in my life.”
This groundbreaking procedure at OHSU not only brings hope to patients suffering from epilepsy and OCD but also emphasizes the importance of collaborative research, innovative thinking, and patient-centered care.
For more science stories check out our New Discoveries section at The Brighter Side of News.
Note: Materials provided above by The Brighter Side of News. Content may be edited for style and length.
Like these kind of feel good stories? Get the Brighter Side of News' newsletter.



