First-of-their-kind wearable sensors continuously monitor health through body sounds
The ability to listen to the intricate symphony of sounds within the human body has long been a vital diagnostic tool.
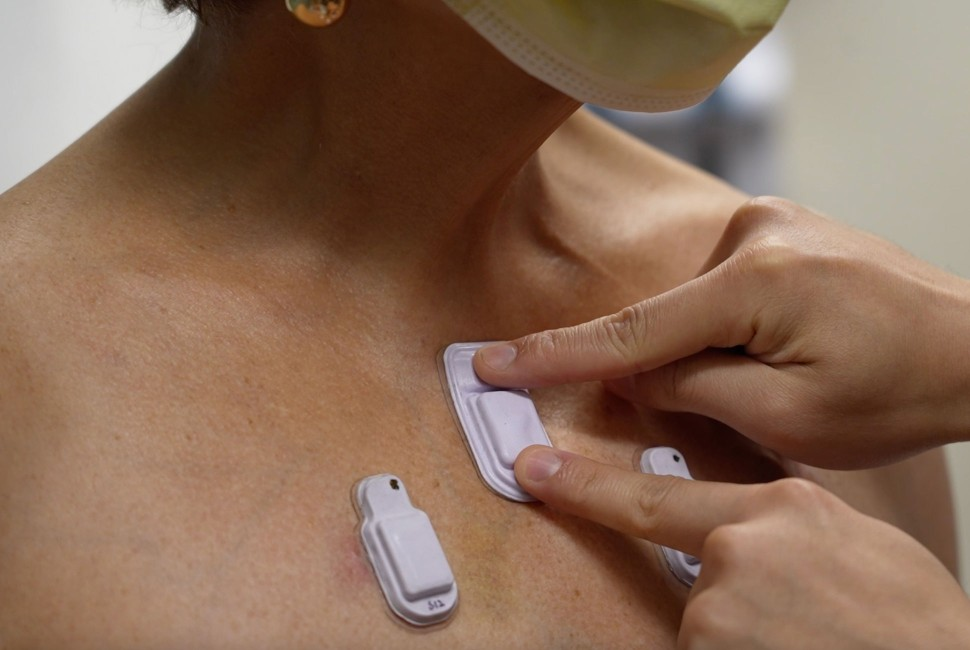
[Nov. 23, 2023: JJ Shavit, The Brighter Side of News]
The ability to listen to the intricate symphony of sounds within the human body has long been a vital diagnostic tool. (CREDIT: Northwestern University)
In the world of medicine, the ability to listen to the intricate symphony of sounds within the human body has long been a vital diagnostic tool. Physicians routinely employ stethoscopes to capture the subtle rhythms of air moving in and out of the lungs, the steady beat of the heart, and even the progress of digested food through the gastrointestinal tract.
These sounds hold valuable information about a person's health, and any deviations from the norm can signal the presence of underlying medical issues. Now, a groundbreaking development from Northwestern University is set to transform the way we monitor these vital sounds.
Researchers at Northwestern University have introduced a revolutionary soft, miniaturized wearable device that transcends the episodic measurements typically obtained during periodic doctor examinations. These innovative devices adhere gently to the skin, enabling continuous, wireless monitoring of crucial body sounds across multiple regions of the body simultaneously. This groundbreaking research was published in the prestigious journal Nature Medicine.
A New Era in Continuous Monitoring
The team behind this transformative technology, led by bioelectronics pioneer John A. Rogers of Northwestern University, recognized the limitations of traditional stethoscopes and sought to develop a more advanced approach.
Related Stories:
Dr. Rogers explained, "Currently, there are no existing methods for continuously monitoring and spatially mapping body sounds at home or in hospital settings. Physicians have to put a conventional, or a digital, stethoscope on different parts of the chest and back to listen to the lungs in a point-by-point fashion. In close collaborations with our clinical teams, we set out to develop a new strategy for monitoring patients in real-time on a continuous basis and without encumbrances associated with rigid, wired, bulky technology."
Dr. Ankit Bharat, a thoracic surgeon at Northwestern Medicine, emphasized the significance of this innovative device, saying, "A key advantage of this device is to be able to simultaneously listen and compare different regions of the lungs. Simply put, it's like up to 13 highly trained doctors listening to different regions of the lungs simultaneously with their stethoscopes, and their minds are synced to create a continuous and a dynamic assessment of the lung health that is translated into a movie on a real-life computer screen."
The Soft Wearable Devices
At the heart of this groundbreaking technology are soft, miniaturized devices that discreetly adhere to the skin. Each device measures 40 millimeters in length, 20 millimeters in width, and 8 millimeters in thickness. Within this compact footprint, the device incorporates a flash memory drive, a tiny battery, electronic components, Bluetooth capabilities, and two miniature microphones—one facing inward toward the body and another facing outward toward the exterior. These dual microphones enable an algorithm to distinguish between external ambient sounds and internal body sounds.
Louis Simpson and Kimberly Querrey Professor of Materials Science and Engineering, Biomedical Engineering, and Neurological Surgery. (CREDIT: Northwestern University)
Dr. Bharat explained, "Lungs don't produce enough sound for a normal person to hear. They just aren't loud enough, and hospitals can be noisy places. When there are people talking nearby or machines beeping, it can be incredibly difficult. An important aspect of our technology is that it can correct for those ambient sounds."
This capability not only allows for noise canceling but also provides critical contextual information about the patient's surroundings, particularly vital when caring for premature babies. Dr. Wissam Shalish, a neonatologist at the Montreal Children's Hospital and co-first author of the paper, highlighted this aspect, stating, "Irrespective of device location, the continuous recording of the sound environment provides objective data on the noise levels to which babies are exposed. It also offers immediate opportunities to address any sources of stressful or potentially compromising auditory stimuli."
The development of these soft wearable devices had two specific vulnerable populations in mind: premature babies in neonatal intensive care units (NICUs) and post-surgery adults. Premature babies, born before or in the earliest stages of the third trimester, often face respiratory challenges as their underdeveloped respiratory systems struggle to adapt to the outside world. Apneas, the cessation of breathing, can be a critical issue for these infants. Current methods of monitoring airflow at the bedside are limited, and accurately distinguishing between apnea subtypes remains a challenge.
Dr. Debra E. Weese-Mayer, a pediatrician and co-author of the study, noted the difficulty in monitoring such tiny patients, saying, "Many of these babies are smaller than a stethoscope, so they are already technically challenging to monitor." The soft acoustic devices offer a solution by continuously and non-invasively tracking a baby's air movement, heart sounds, and intestinal motility, both during wakefulness and sleep. This continuous monitoring provides invaluable data to clinicians, allowing for a deeper understanding of each infant's unique health patterns.
When placed on the abdomen, the automatic detection of reduced bowel sounds could alert the clinician of an impending (sometimes life-threatening) gastrointestinal complication. (CREDIT: Northwestern University)
Collaborative studies conducted at the Montreal Children's Hospital demonstrated the effectiveness of these devices in NICU settings. Placed just below the suprasternal notch at the base of the throat, the devices accurately detected airflow and chest movements, enabling the identification and classification of all apnea subtypes. Dr. Shalish highlighted the potential benefits, stating, "When placed on the right and left chest of critically ill babies, the real-time feedback transmitted whenever the air entry is diminished on one side relative to the other could promptly alert clinicians of a possible pathology necessitating immediate intervention."
A Revolutionary Approach to Monitoring Digestion
In addition to their role in neonatal care, these soft wearable devices also hold promise in monitoring the digestive health of infants and children. Cardiorespiratory and gastrointestinal problems are leading causes of mortality in the first five years of life, and reduced bowel sounds can be an early indicator of digestive issues, intestinal dysmotility, and potential obstructions. The pilot study in the NICU involved placing sensors on premature babies' abdomens, and early results aligned with wire-based systems used in adult patients.
When placed on the abdomen, the automatic detection of reduced bowel sounds could alert the clinician of an impending (sometimes life-threatening) gastrointestinal complication. (CREDIT: Northwestern University)
Dr. Shalish emphasized the potential significance of this aspect, saying, "When placed on the abdomen, the automatic detection of reduced bowel sounds could alert the clinician of an impending (sometimes life-threatening) gastrointestinal complication." Dr. Weese-Mayer added, "Intestinal motility has its own acoustic patterns and tonal qualities. Once an individual patient's acoustic 'signature' is characterized, deviations from that personalized signature have potential to alert the individual and health care team to impending ill health, while there is still time for intervention to restore health."
Transforming Adult Healthcare
Accompanying the NICU study, researchers also conducted tests on adult patients, including those with chronic lung diseases and healthy controls. The devices captured the distribution of lung sounds and body motions simultaneously at various locations, providing a comprehensive analysis of a single breath across different regions of the lungs.
The introduction of soft, miniaturized wearable devices for continuous monitoring of body sounds represents a significant leap forward in healthcare. (CREDIT: Northwestern University)
Dr. Bharat highlighted the significance of this development in the context of respiratory diseases, which claimed nearly 800,000 lives in the U.S. in 2020, according to the Centers for Disease Control and Prevention. He said, "Lungs can make all sorts of sounds, including crackling, wheezing, rippling, and howling. It's a fascinating microenvironment. By continuously monitoring these sounds in real time, we can determine if lung health is getting better or worse and evaluate how well a patient is responding to a particular medication or treatment. Then we can personalize treatments to individual patients."
The introduction of soft, miniaturized wearable devices for continuous monitoring of body sounds represents a significant leap forward in healthcare. These devices have the potential to revolutionize the way clinicians diagnose and treat a wide range of medical conditions, from respiratory disorders to gastrointestinal problems. With their ability to provide real-time data and their non-invasive nature, they offer a promising future for improving patient outcomes and saving lives. As technology continues to advance, we can anticipate even more innovative solutions that will further enhance the capabilities of these remarkable devices
Wireless networks of BAMS systems and their use in simultaneous spatiotemporal mapping of lung sounds and chest wall movements. (CREDIT: Nature)
John A. Rogers holds the Louis Simpson and Kimberly Querrey Professorship in Materials Science and Engineering, Biomedical Engineering, and Neurological Surgery at Northwestern's McCormick School of Engineering and Feinberg School of Medicine. He also directs the Querrey Simpson Institute for Bioelectronics. Dr. Ankit Bharat serves as the Chief of Thoracic Surgery and holds the Harold L. and Margaret N. Method Professorship of Surgery at Feinberg.
As the director of the Northwestern Medicine Canning Thoracic Institute, Dr. Bharat made history by performing the first double-lung transplants on COVID-19 patients in the U.S. and initiating a pioneering lung transplant program for certain patients with stage 4 lung cancers.
Note: Materials provided above by the The Brighter Side of News. Content may be edited for style and length.
Like these kind of feel good stories? Get the Brighter Side of News' newsletter.