Inside the neural implant letting paralyzed patients type at 110 characters per minute
Researchers have built a brain implant that restores typing for paralyzed users at speeds rivaling able-bodied performance.

 Edited By: Joseph Shavit
Edited By: Joseph Shavit
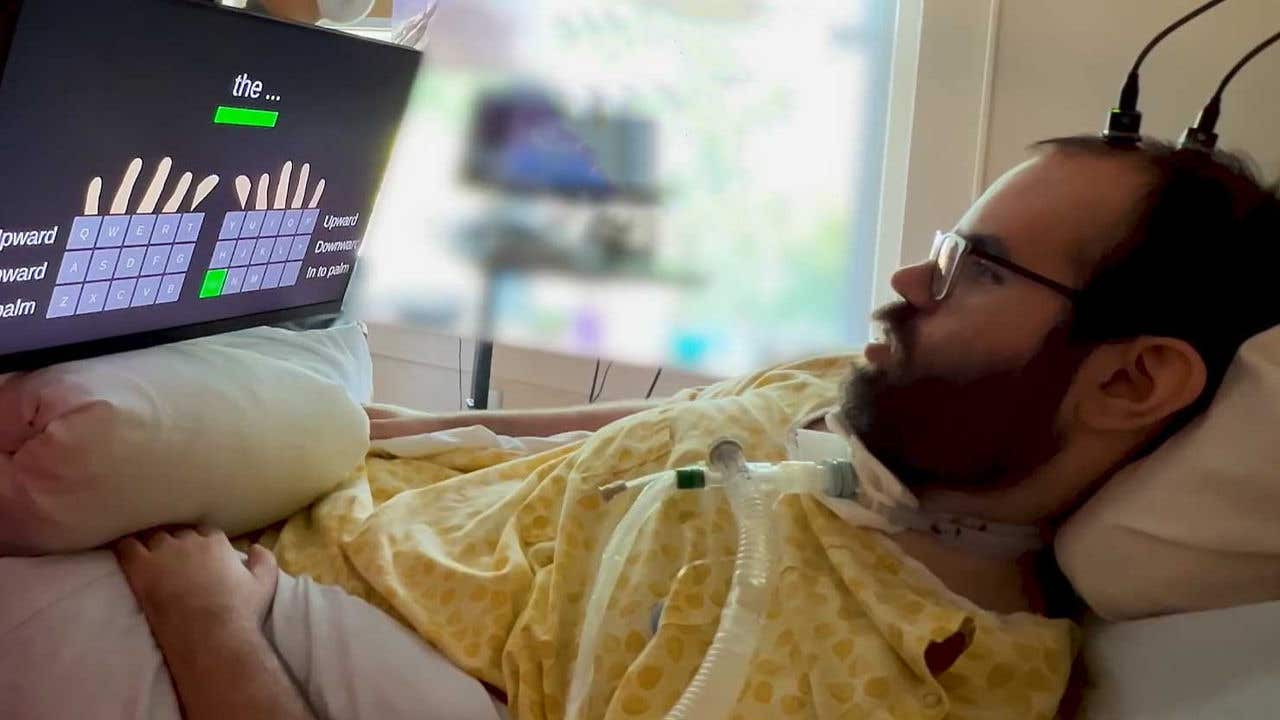
An implantable device researched by Mass General Brigham investigators and colleagues allows communication through rapid typing for a person with ALS and a person with a spinal cord injury. (CREDIT: Mass General Brigham)
Before his disease took his voice, he could type a message as fast as anyone. Now, with electrodes no larger than a grain of rice embedded near the surface of his brain, he can do it again, at 110 characters per minute, with an error rate that would make most smartphone users envious.
That's the core of what researchers from Mass General Brigham Neuroscience Institute and Brown University are reporting in Nature Neuroscience: a brain-computer interface that lets people with paralysis type using a standard QWERTY keyboard, not by moving their hands, but by simply attempting to. The system interprets the brain's intention to move specific fingers and translates those signals into letters, in real time, with no physical movement required.
Two participants tested the device as part of the BrainGate2 clinical trial. One has amyotrophic lateral sclerosis, a progressive disease that attacks the nerve cells controlling movement and speech. The other has a cervical spinal cord injury. Both used the system from their homes, not a research lab, a detail the team considers significant.
The Problem This Solves
For people with paralysis affecting both their hands and their speech, communication options have long been frustrating at best. Eye-gaze systems, which track where a person looks to select letters one at a time, are among the most widely used alternatives. They work, but slowly. Users report fatigue, frequent recalibration requirements, and a grinding, letter-by-letter pace that can turn a simple sentence into a minutes-long ordeal.
"For many people with paralysis, when losing use of both the hands and the muscles of speech, communication can become difficult or impossible," said senior author Daniel Rubin, MD, PhD, a critical care neurologist at Mass General Brigham. "Patients often find this and other types of augmentative and alternative communication systems frustrating to use. BCIs are on track to become an important new alternative to what's currently offered."
High abandonment rates in existing devices aren't a minor inconvenience. They represent a near-total loss of voice for people who still have things to say.
How the Brain Learns to Type Again
The implanted system works through microelectrode arrays placed in the motor cortex, the brain region responsible for planned and executed movement. The QWERTY layout is displayed on a screen in front of the user. Each key is mapped to a specific finger and one of three positions: extending upward, pressing straight down, or curling into the palm. Those three movements per finger, across ten fingers, cover all 26 letters plus a space and basic punctuation, 30 distinct tokens in total.
As the participant attempts the corresponding finger movement, even without any actual physical motion, the electrodes pick up the brain's electrical signals. A recurrent neural network interprets those signals as characters in sequence, and a language model refines the output into coherent words and sentences. The whole process happens continuously and at a pace set entirely by the user.
Neither participant was a touch typist before their illness or injury. Both improved steadily across sessions.
The faster of the two, identified in the study as participant T18, who has a spinal cord injury, reached 110 characters per minute with a word error rate of 1.6 percent, performance the authors describe as comparable to able-bodied typing accuracy. The participant with ALS, T17, reached 47 characters per minute. That's slower, but still far faster than what most eye-gaze users can achieve.
One of the more striking findings involves calibration. T18 needed as few as 30 sentences to get the system up and running. Earlier brain-computer interface approaches, including those based on decoding imagined handwriting, required more training data to reach usable accuracy.
Why QWERTY, Specifically
The choice of a standard keyboard layout wasn't incidental. Most people who develop paralysis later in life, after years of typing on phones and computers, already carry a mental map of where letters sit. That familiarity matters. The brain retains those movement patterns even when the body can no longer execute them.
There's also a technical advantage. With handwriting decoding, the errors that creep in tend to cluster around similarly shaped letters, things like the curve of an "a" versus an "e," letters that also happen to be interchangeable in common English words. QWERTY errors, by contrast, occur mostly between neighboring keys, which are far less likely to substitute cleanly for one another in real language. The language model catches more of those errors as a result.
"Decoding these finger movements is also a big step toward being able to restore complex reach and grasp movements for people with upper extremity paralysis," said first author Justin Jude, PhD, a postdoctoral researcher at Mass General Brigham. "And there's also room to make this communication tool better, like implementing a stenography or otherwise personalized keyboard to make typing even faster."
What Remains Uncertain
The study involved two participants. That's a small number, and the researchers acknowledge it. The two participants also differ in meaningful ways, including the nature of their conditions, the number of electrodes implanted, and where those electrodes were placed. T18 had 384 electrodes across both brain hemispheres; T17 had 128, all on one side. Those differences likely account for some of the gap in their respective typing speeds and error rates.
Neural signals also drift over time. The team found that a decoder trained on one day's data started degrading in accuracy after several days without recalibration, though the drop-off was gradual enough that one-day-old training still produced usable results. Future versions of the system will aim to update the decoder automatically during normal use, eliminating the need for scheduled recalibration sessions.
Co-author Leigh Hochberg, MD, PhD, who leads the BrainGate clinical trial, placed the work in a longer arc. "Since 2004, our BrainGate team has been advancing and testing the feasibility and efficacy of implantable brain computer interfaces to restore communication and independence for people with paralysis," he said. "The BrainGate consortium demonstrates the strength of academic and university-based researchers working together, thinking about what's possible, and then advancing the frontiers of restorative neurotechnology."
Practical Implications
For people living with advanced ALS, severe spinal cord injuries, brainstem strokes, or other conditions causing locked-in or near-locked-in states, the implications of faster, more accurate communication tools are difficult to overstate. Existing assistive technologies often fail precisely the people who need them most; some users with advanced ALS cannot reliably operate eye-gaze systems at all.
A device that allows typing at speeds approaching normal text communication, from home, without a care partner present for constant recalibration, would change the day-to-day reality of what those individuals can do and who they can reach. The team envisions future versions of the system connecting directly to email, messaging apps, and text-to-speech output.
The keyboard itself may also evolve. The researchers are planning to add wrist gestures that would switch between character sets, numbers, different alphabets, special keys like Shift and Backspace, and accommodations for passwords and character strings that don't follow standard English patterns. The bones of the system are already there. What comes next is making it fast enough, flexible enough, and independent enough to live outside a clinical trial.
Research findings are available online in the journal Nature Neuroscience.
The original story "Inside the neural implant letting paralyzed patients type at 110 characters per minute" is published in The Brighter Side of News.
Related Stories
- New brain-computer interface turns silent thoughts into words
- Noninvasive brain scanning could restore movement after spinal cord injury
- Wireless implant sends information straight to the brain using light
Like these kind of feel good stories? Get The Brighter Side of News' newsletter.
Mac Oliveau
Writer
Mac Oliveau is a Los Angeles–based science and technology journalist for The Brighter Side of News, an online publication focused on uplifting, transformative stories from around the globe. Passionate about spotlighting groundbreaking discoveries and innovations, Mac covers a broad spectrum of topics including medical breakthroughs, health and green tech. With a talent for making complex science clear and compelling, they connect readers to the advancements shaping a brighter, more hopeful future.



