Self-swabs for COVID-19 comparable to in-clinic detection
[July 25, 2020: University of Washington Medicine] A small-scale study suggests that, among people with high viral loads, self-collected…
[July 25, 2020: University of Washington Medicine]
A small-scale study suggests that, among people with high viral loads, self-collected swabs of the midnasal area are comparable to swabs administered by healthcare workers in their ability to detect the virus that causes COVID-19.
The findings are reported in a research letter published today in JAMA Network Open. The lead author is Dr. Denise J. McCulloch, an infectious disease fellow of medicine at the University of Washington School of Medicine. Dr. Helen Y. Chu, a UW professor of medicine, Division of Allergy and Infectious Diseases, was senior author.
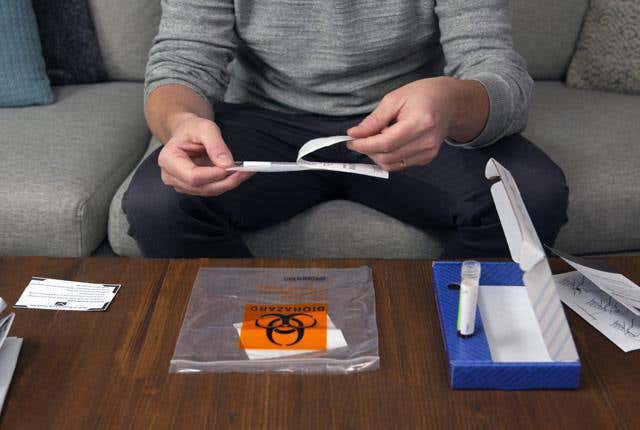
There are advantages to at-home self-swabs that are sent to a lab for SARS-CoV-2 testing: Patients avoid going out when they don’t feel well, which reduces potential contagion and saves healthcare workers’ protective equipment and supplies. It also gives public health officials a means to track the pandemic in communities among people who don’t seek care at hospitals, clinics, and test sites.
The study involved 185 participants who provided samples via clinician-collected nasopharyngeal swab, self-collected midnasal swab, or both. (With midnasal swabs, people insert the swab about 1 inch into the nose. The clinically administered nasopharyngeal swab goes much farther back, depending on the patient’s anatomy, toward the nasal pathway opening to the throat.)
Among the participants, 41 (22.2%) tested positive for SARS-CoV-2. The home midnasal-swab collection was comparable to clinician-collected nasopharyngeal samples for detecting the novel coronavirus in symptomatic patients.
Compared with swabs collected in clinic – the gold-standard diagnostic approach – the diagnostic sensitivity of the home swabs was 80%; that is, the home swabs correctly identified 80% of the positive cases detected by in-clinic swabs. Among people infected with “meaningful” viral loads, the home swabs did even better, detecting 95% of those cases, said Chu.
“It matters less if swabs don’t detect the cases with very little virus, because they’re not likely to be very symptomatic and less likely to infect others,” Chu added.
The home swabs’ specificity was 97.9% – lower than that described in previous studies done in clinic. Specificity is the ability to correctly identify those who do not have the disease, or the true negatives. Chu attributed the home swabs’ lower specificity to participants with low viral loads and to the fact that most participants self-administered the home swabs a day after they had been tested by a clinician, so their viral loads were lower.
Like these kind of stories? Get The Brighter Side of News' newsletter!
Programs providing home self-collected swab kits may improve testing accessibility at a time when more diagnostics are urgently needed to contain the rising spread of the pandemic. As several states reopen businesses, schools, and recreation sites, the researchers believe that expansion of COVID-19 testing is critical to managing the pandemic.
Before such efforts are expanded, however, researchers must ensure that home self-swabs are comparable to clinician-swabs, and limit the percentage of false-negative and false-positive readings.
The researchers outlined some of the study’s limitations. Shipping without temperature controls could have contributed to sample degradation. Previous studies, however, showed that samples could remain stable at ambient temperature for up to nine days. Also, many of the study participants were healthcare professionals, and their swabbing ability may have differed from that of the general public. Finally, using clinician-collection swabs as the standard may have introduced bias.
The researchers proposed that home-based strategies should try to reach individuals in the early stages of illness, when they are more likely to transmit the disease to others and less likely to seek medical care until symptoms worsen.
“Home swab collection,” they said, “has the potential to play a pivotal role in increasing testing access across the broader population.”
Other researchers on the study were Ashley E. Kim, Naomi C. Wilcox, and Jennifer K. Louge of the Chu lab, Alex L. Greninger of the Division of Virology, Department of Laboratory Medicine and Pathology of the UW School of Medicine, and Janet A. Englund of the Department of Pediatrics, UW School of Medicine and of Seattle Children’s Hospital.
The study was supported by Gates Ventures.
MEDIA CONTACT:
Brian Donohue - 206.543.7856, bdonohue@uw.edu



