Best evidence yet that lowering blood pressure can prevent dementia
A global study has provided the strongest evidence to date that lowering blood pressure in later life can cut the risk of dementia.
[Oct 27, 2022: Tina Wall, George Institute for Global Health]
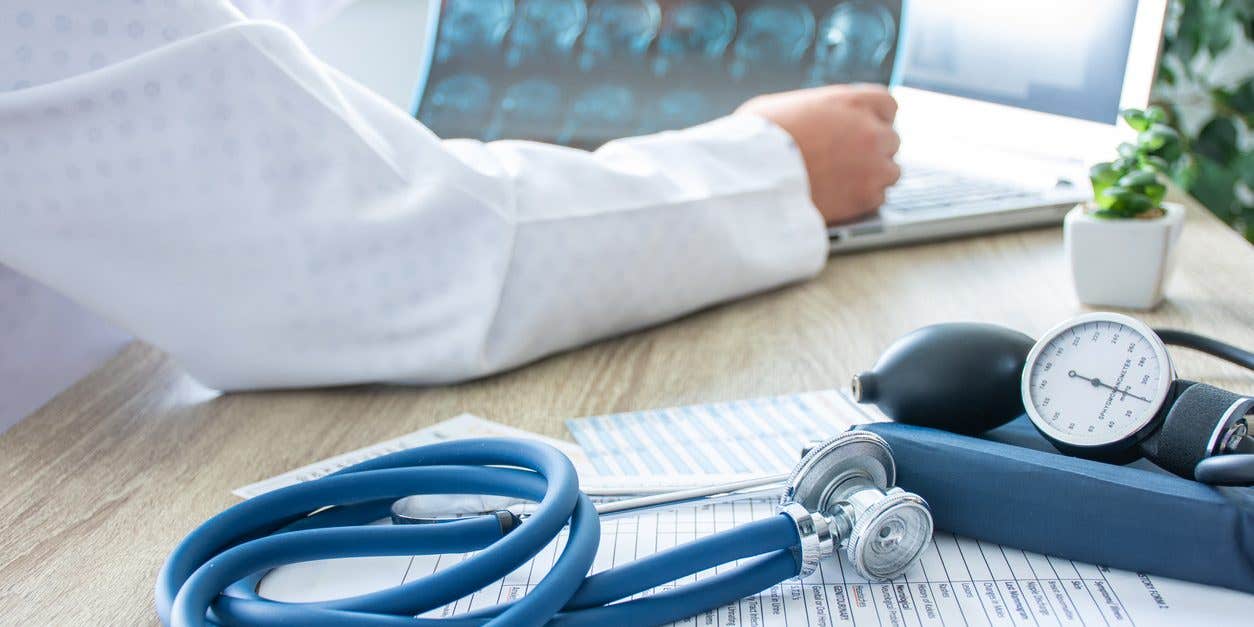
A global study of over 28,000 people has provided the strongest evidence to date that lowering blood pressure in later life can cut the risk of dementia. (CREDIT: Creative Commons)
A global study of over 28,000 people has provided the strongest evidence to date that lowering blood pressure in later life can cut the risk of dementia.
Dr Ruth Peters, Associate Professor at UNSW Sydney and Program Lead for Dementia in The George Institute’s Global Brain Health Initiative, said that in the absence of significant dementia treatment breakthroughs, reducing the risk of developing the disease would be a welcome step forward.
“Given population ageing and the substantial costs of caring for people with dementia, even a small reduction could have considerable global impact,” she said.
“Our study suggests that using readily available treatments to lower blood pressure is currently one of our ‘best bets’ to tackle this insidious disease.”
Dementia is fast becoming a global epidemic, currently affecting an estimated 50 million people worldwide. This is projected to triple by 2050 - mainly driven by aging populations.
Related Stories
It is currently estimated to cost US$20-$40,000 per person with the condition each year.
Dr Peters explained that while many trials have looked at the health benefits of lowering blood pressure, not many included dementia outcomes and even fewer were placebo-controlled – considered to provide the best level of evidence.
“Most trials were stopped early because of the significant impact of blood pressure lowering on cardiovascular events, which tend to occur earlier than signs of dementia,” she said.
To examine the relationship between blood pressure and dementia more closely, researchers analysed five double-blind placebo-controlled randomised trials that used different blood pressure lowering treatments and followed patients until the development of dementia.
A total of 28,008 individuals with an average age of 69 and a history of high blood pressure from 20 countries were included. Across these studies, the mid-range of follow up was just over four years.
“We found there was a significant effect of treatment in lowering the odds of dementia associated with a sustained reduction in blood pressure in this older population,” said Dr Peters.
“Our results imply a broadly linear relationship between blood pressure reduction and lower risk of dementia, regardless of which type of treatment was used.”
Researchers hope the results will help in designing public health measures to slow the advance of dementia as well as informing treatment, where there may be hesitations around how far to lower blood pressure in older age.
“Our study provides the highest grade of available evidence to show that blood pressure lowering treatment over several years reduces the risk of dementia, and we did not see any evidence of harm,” said Dr Peters.
Class I evidence in favour of antihypertensive treatment reducing risk of incident dementia compared with placebo. (CREDIT: European Heart Journal)
“But what we still don’t know is whether additional blood pressure lowering in people who already have it well-controlled or starting treatment earlier in life would reduce the long-term risk of dementia,” she added.
Professor Craig Anderson, Director of the Global Brain Health program at The George Institute said, “this work is an important foundation for clinical trials to provide reliable estimates of the benefits and risks of preventative treatments, and how best to apply them across different populations.”
For more science and technology stories check out our New Discoveries section at The Brighter Side of News.
Note: Materials provided above by George Institute for Global Health. Content may be edited for style and length.
Like these kind of feel good stories? Get the Brighter Side of News' newsletter.



